Modules 3 & 4: Biological Models of Addiction
Ch. 4: More about Neurotransmitters and How Neurons Communicate
It is helpful to take a closer look at what happens at the level of neurons and their communication with each other through neurotransmitters. This is relevant because the psychotropic effects of the substances we are studying are very often related to the impact these substances have at the level of neurotransmission.
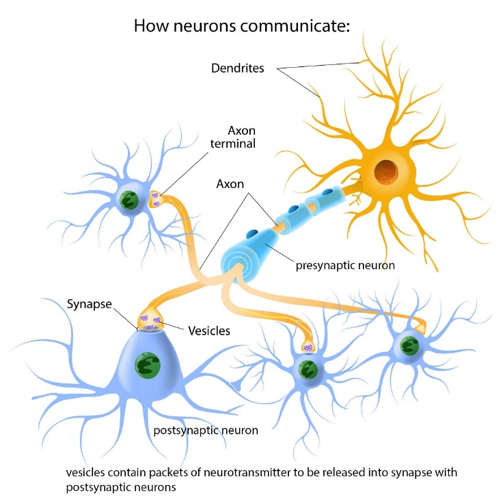
Figure 1 shows the layout of what happens when brain neurons in close physical proximity to each interact or communicate. It makes sense to consider this microscopic level because these are the building blocks of the brain regions that play a role in how substance use can become a substance use disorder. The neurotransmitters that you have been reading about are contained in packets called vesicles, located in the terminal area of a neuron’s axon—the area that comes into close contact with the neighboring neurons. The space between the neurons is the synapse, or synaptic cleft. And this space between neurons is where those neurotransmitters are released to work their changes on their neighboring neurons. The “sending” neuron is the presynaptic neuron, while the receiving neuron is the postsynaptic neuron.
Figure 1.
Several neurotransmitters are known to play a role in the development, maintenance, and recovery from alcohol or other substance use disorders, as well as other forms of addiction. These include:
Several things are very important to understand about neurotransmitters and the system of communication in which they are involved:
- Each type of neurotransmitter is concentrated in one or more specific regions of the brain—they are not distributed evenly all over the brain.
- We used to believe that a neuron could only release one type of neurotransmitter. More recent research indicates that in many cases the same neuron can release two and possibly more types depending on the frequency of the stimulation its receives—at one frequency it might release one type of neurotransmitter, at another frequency it might release a different type.
- Most neurotransmitters occur naturally as important chemicals in other parts of the body (including the peripheral nervous system and other organs) where they have other health-related functions, not just in the brain (central nervous system).
- Neurotransmitter release is triggered by many natural behaviors, not just by drugs. For example, dopamine release is involved in the natural reward systems associated with food, sex, humor, pair-bonding (mates), listening to music, video games. The addictive potential of a psychotropic drug increases when the concentration of dopamine released is higher compared to what is released by natural behaviors (Johnson, 2014).
- Fast uptake of a drug, for example getting it to the brain by injection rather than ingesting it orally, produces a stronger “high” and therefore a greater potential for addiction. This is because more dopamine is released at once, so it is more powerfully rewarding (Volkow et al., 2010).
- Neurotransmitters released by the presynaptic neuron must be received by their specific receptors on a postsynaptic neuron. If the postsynaptic neuron does not have the right receptors, the release of the neurotransmitter into the synapse/synaptic cleft between them has no effect.
- The brain has specific receptors for certain substances (like the cannabinoid or opioid receptors) because there are endogenous forms of these or chemically similar substances. An example are the naturally occurring enkephalins that bind to the body’s opioid receptors, similar to how endorphins work.
- Transporters return the “spent” neurotransmitter substances back to the original (presynaptic) neuron to prepare for release again in the future. Transporters serve to clean up and reduce the concentration of the neurotransmitter in the synaptic space/cleft.
- Neurotransmitters tend to be either excitatory or inhibitory in nature, although a few can do both/either function (an example is dopamine). Excitatory neurotransmitters turn “on” or stimulate a neuron to fire, inhibitory neurotransmitters turn “off” or block a neuronl from firing.
- Agonist substances trigger a receptor to produce a response, because the receptors “recognize” and bind to it. For example, the THC in marijuana (cannabis) is an agonist that activates the cannabinoid receptors.
- Antagonist substances prevent a receptor from producing its response by blocking the binders or otherwise preventing the response. For example, naloxone treats a heroin/opioid overdose by blocking the effects of the drugs on the body’s opioid receptors.
- Certain substances, when combined, create a stronger neurotransmitter response than either could alone. This is called potentiation.
Neurotransmitters and Withdrawal
At this point, you have developed a basic understanding of how neurotransmitters play a role in substance use, and have come to recognize the names of some of the key players. Let’s take a brief look at the other side of the coin: how neurotransmitters play a role in the experience of withdrawal from certain substances and why this might make a difference in keeping a person motivated to maintain a “quit” attempt after developing a substance use disorder. Here, we can draw from content presented in articles published by Koob and Simon (2009) and Trevisan et al (1998). They tell us that:
- A decrease in dopamine or serotonin (as well as something called the opioid peptide) contributes to the experience of dysphoria. What is dysphoria? Dysphoria is the experience of a profound sense of unease, unhappiness, and general dissatisfaction, often associated with major depression and anxiety. [Your other readings also talked about the experience of anhedonia during recovery/prolonged withdrawal, as you may recall. The idea is the same: it is a punishing emotional/psychological experience.]
- A decrease in GABA contributes to the experience of anxiety, even panic attacks, due to the resulting nervous system hyperactivity.
- An increase in norepinephrine contributes to the experience of stress.
- An increase in glutamate contributes to hyperexcitability.
Why does this matter? Because these negative emotional and psychological states make it difficult to sustain one’s motivation to avoid taking drugs and contribute to the pressure a person might feel to relapse back to using again. And, depending on the nature of the substances involved, withdrawal may lead to decreased dopamine, serotonin, or GABA, as well as increased norepinephrine or glutamate. Knowing about these links between neurotransmitter changes during prolonged withdrawal from using a substance has contributed to the development of several medications to help manage these negative experiences; this, in turn, may help a person to sustain a quit attempt over time. (We will learn more about these medications in Module 13 when we study pharmacotherapy strategies.) Another reason why all of this matters: it helps us to understand the biology behind the frequently reported observation that, during withdrawal and early recovery from many types of substances, the risk for suicide is greater than in the general population.
Interactive Exercise:
See if you can complete this picture laying out how neurons in the brain interact and communicate–refer back to Figure 1 above for the answers.
