Chapter 10: Respiratory System
Air conduction: Larynx, Trachea, Bronchi and Bronchioles
Larynx
The larynx is a complex, tubular organ, the structure of which is primarily composed of elastic and hyaline cartilage and skeletal muscle. The larynx connects the naso- and oro-pharynx with the trachea, functioning in air conduction, vocalization, and in obstructing passage of ingesta into the trachea during deglutition. The epithelium of the larynx is variable, but is generally stratified squamous epithelium in the rostral segment proximal to the pharynx, and ciliated pseudostratified columnar (respiratory) epithelium elsewhere. The lamina propria subjacent to the laryngeal epithelium contains secretory glands.
Trachea, bronchi and bronchioles
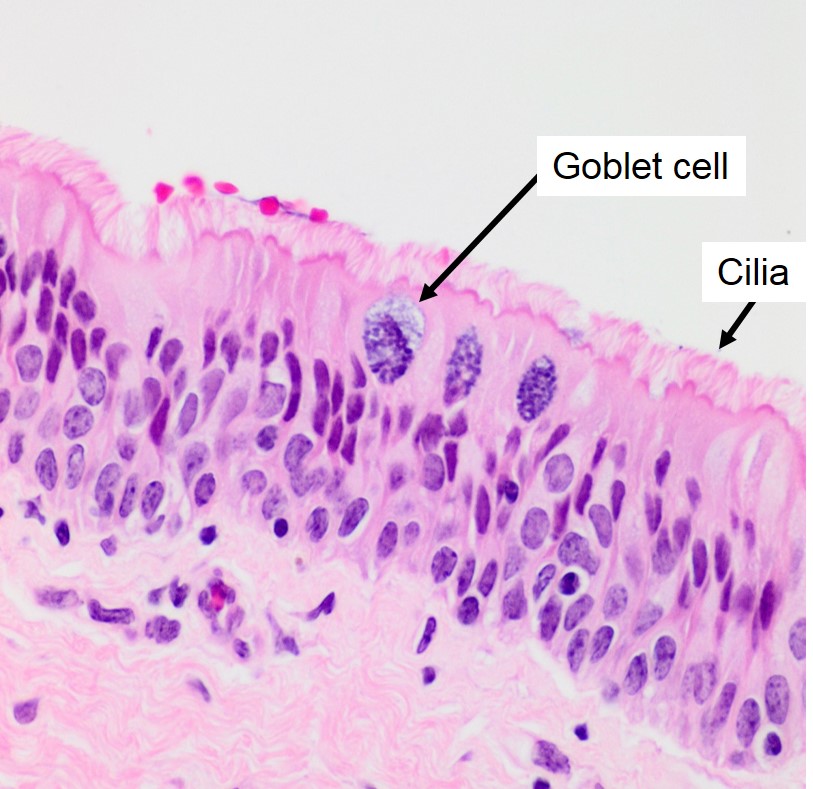
The luminal (mucosal) surface of the trachea is lined by ciliated, pseudostratified columnar epithelium (i.e. respiratory epithelium) interspersed with goblet cells. The lamina propria and submucosa also contain small mixed (mucous and serous) glands and smooth muscle. The trachea is supported by a series of C-shaped cartilaginous (hyaline cartilage) rings. Dorsally, the ends of the incomplete cartilaginous rings of the trachea are connected by a band of smooth muscle: the trachealis muscle. Externally, the trachea is surrounded by a thin layer of fibrovascular connective tissue (adventitia).
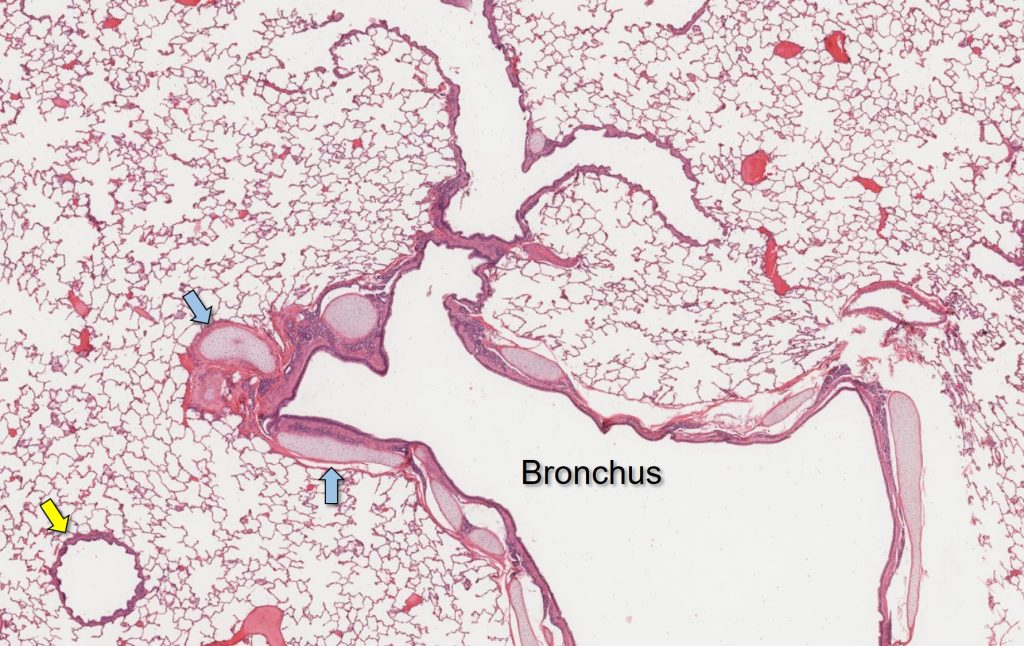
Distally, the trachea divides into the left and right mainstem bronchi. Bronchi are histologically similar to the trachea. They are lined by ciliated, pseudostratified columnar epithelium (respiratory epithelium) and interspersed with goblet cells. The walls of bronchi are also supported by cartilage and smooth muscle.
The smooth muscle of airways mediates bronchoconstriction, the process of contraction and subsequent narrowing of the airway lumen. Bronchoconstriction is mediated, in part, via mast cell-derive histamine, and bronchoconstriction is a life-threatening effect of massive histamine release (e.g. anaphylaxis). Finally, the lamina propria of bronchi also contain moderate numbers of mixed glands (bronchial glands). These are particularly abundant in cats. As the bronchi extend deep into the pulmonary parenchyma, they continue to bifurcate, giving rise to smaller caliber (diameter) secondary and tertiary bronchi.
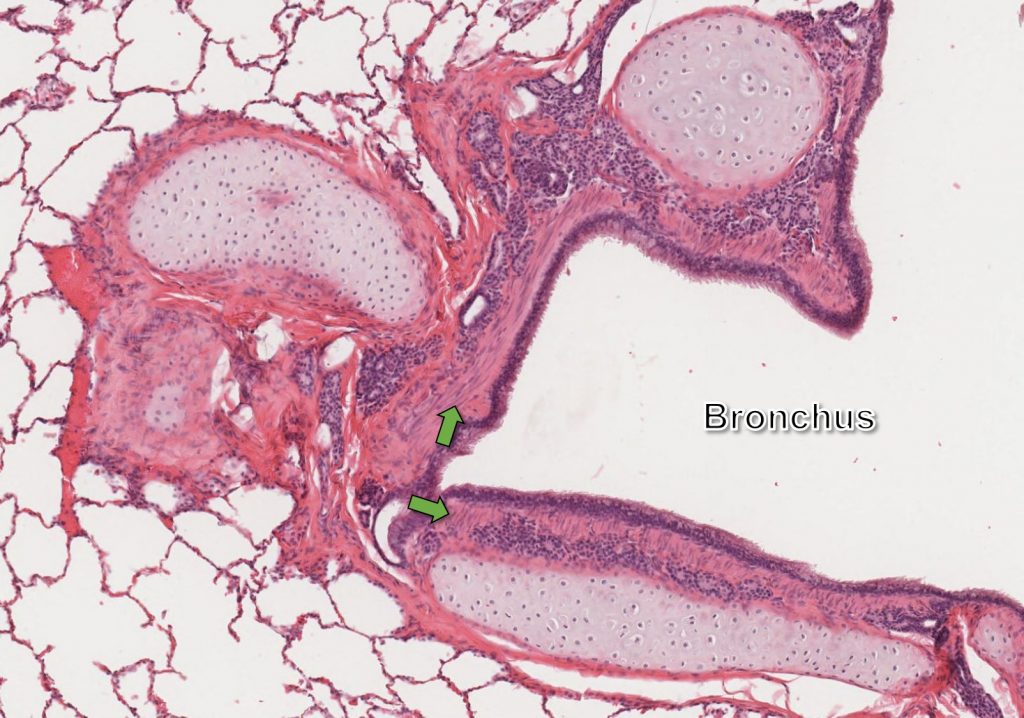
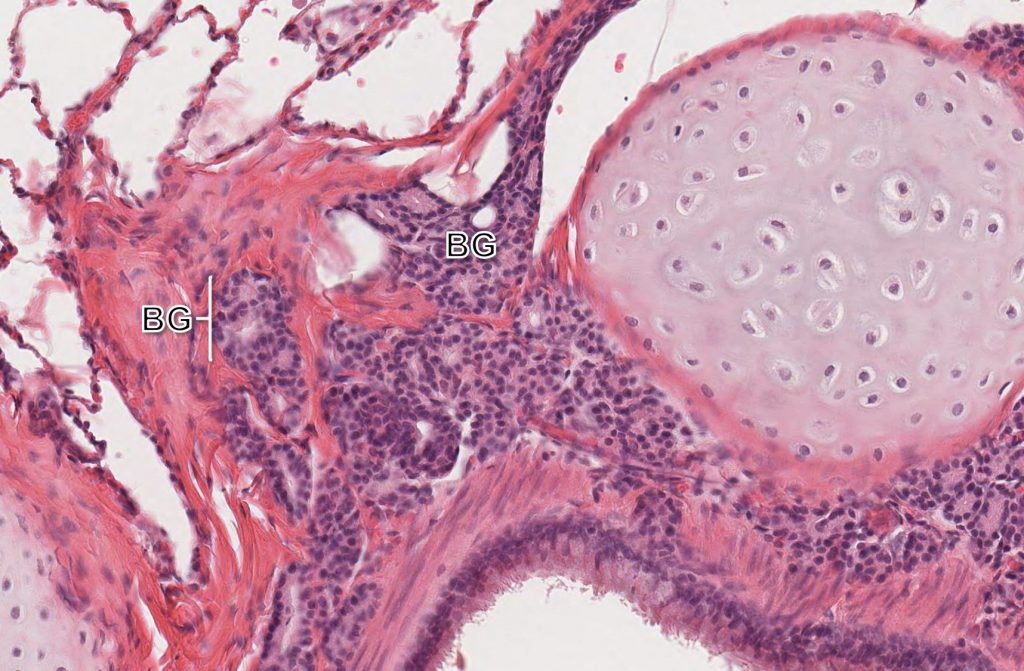
Eventually, bronchi give way to smaller conducting airways, bronchioles. Bronchioles are thin-walled airways lined by variably ciliated or non-ciliated columnar epithelium. The walls are composed of tangentially arranged smooth muscle. Bronchioles lack cartilage and glands which, along with their smaller size, distinguish them histologically from bronchi.
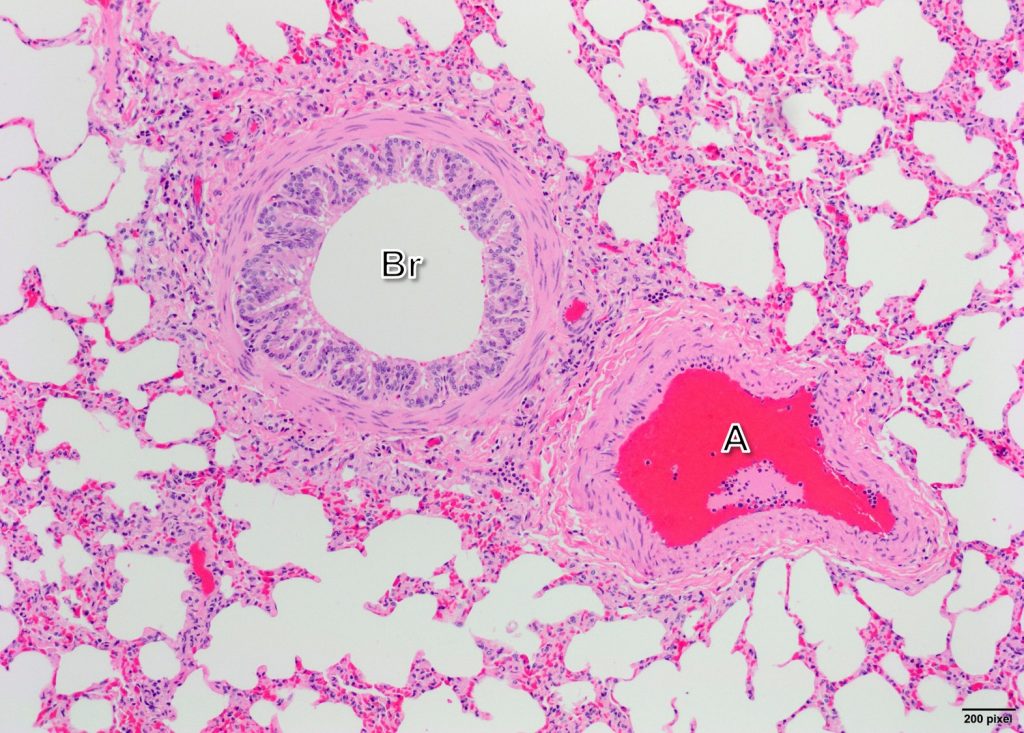
The transition between regions of air conduction (i.e. bronchioles) and regions of air exchange (i.e. alveoli) in the lung progresses through sequentially distinct segments; from proximal to distal: terminal bronchioles, respiratory bronchioles, alveolar ducts, alveolar sacs, and alveoli.
